Dos and Don’ts After Laparoscopy
Laparoscopic surgery is a minimally invasive procedure that helps your general surgeon in Navi Mumbai take a deeper look at your internal organs, get the most accurate diagnosis, and figure out a viable treatment plan.
Laparoscopy can be used for diagnosis and treatment. For instance, it can give your surgeon a clear picture of the uterine fibroids while also removing them through several small incisions on your abdomen. The question is, what does recovery look like, and what can you do after laparoscopy to speed up your recovery? Let’s take a look at the several dos and don’ts after laparoscopy.
Dos and Don’ts After Laparoscopy
Dos After Laparoscopy
i) Follow Your Doctor’s Instructions:
Your surgeon will explain post-operative instructions, such as when to wash the incision site, when to start walking, how much physical activity is safe, the medication you should take, and when to see your doctor. Follow their instructions carefully.
ii) Maintain a Balanced Diet:
Eat a diet rich in essential vitamins, minerals, fiber, omega-3 fatty acids, and other nutrients to maintain your energy levels. If you experience stomach ache or gas, switch to bland, low-fat food. Drink enough fluids to maintain hydration.
iii) Engage in Light Physical Activity:
Rest is the key to fast recovery, but that doesn’t mean you need to go into bed rest. Light activity, such as a stroll in your street or gentle stretching a few days after the surgery, can help promote blood circulation, prevent blood clots, and speed up your recovery.
iv) See Your Doctor:
Visit the surgery hospital in Navi Mumbai for your follow-up appointments. Your surgeon will assess your incision and your overall health to ensure you are in good health and recovering normally.
Don’ts After Laparoscopy
a) Avoid Heavy Lifting:
Do not push yourself beyond your limits. While it’s normal to want a quick recovery and to want to get back to your routine life soon after surgery, strenuous exercises must be avoided. Likewise, heavy lifting, including carrying grocery bags, suitcases, pets, and babies, is off-limits.
b) Refrain From Driving Immediately:
Arrange your drive back home after surgery. Driving is usually restricted until you are on pain meds. Besides, sitting for prolonged hours can strain your abdomen.
c) Don’t Neglect Signs of Complications:
See your doctor immediately if you have a high-grade fever that persists for days with swelling and discharge from the incision site. Other signs of complications include severe pain that doesn’t subside with pain-relieving medication, nausea, vomiting, and difficulty breathing.
Tips for a Smooth Recovery
Here’s what you can do to achieve fast recovery:
- Practice light physical activity
- Use a pillow for abdominal support when laughing, sneezing, or coughing
- Avoid household chores until your doctor clears you for it.
- Watch out for unusual signs and seek immediate medical assistance
- Get ample rest
Conclusion
While there’s a general recovery timeline for laparoscopy, every patient has their own recovery journey. Your progress after the procedure depends on the hospital, the doctor’s expertise, the nursing staff, your pain tolerance, the duration of the surgery, and other factors.

Signs and Symptoms of a Fracture
A crack in your bone due to trauma or stress can lead to a fracture. People diagnosed with osteoporosis and bone cancer are also at an increased risk of developing fractures. Depending on the severity of the trauma, a fracture could be closed (the bone cracks but doesn’t break through your skin) or comminuted (the bone breaks into multiple pieces). If you suspect a fracture, get to the nearest orthopedic hospital in Navi Mumbai for the best care.
Common Causes of Fractures
i) Accidents and falls:
Healthy bones are strong enough to withstand pressure effortlessly. However, if you experience a serious fall or an accident that puts a great deal of force on your bones, they might break.
ii) Sports injuries:
Sports that require a lot of twisting and turning can cause fractures. People involved in sports can develop spiral, transverse, comminuted, hairline, and stress fractures.
iii) Osteoporosis and bone weakening conditions:
With age, your bone density and resilience decrease significantly, making you more prone to sustaining a fracture even with low-impact trauma.
Signs and Symptoms of a Fracture
a) Pain and tenderness:
Intense pain on the injured site is the hallmark symptom of a fracture. It’s your body’s way of telling you that something isn’t right and requires medical attention. People with fractures might feel pain when touching the site, moving it, or putting weight on it. It may not get better with rest.
b) Swelling and bruising:
The tissue damage can cause swelling, which won’t go down. You might also notice bruising (your skin turning blue, purple, or yellow) that indicates bleeding under your skin.
c) Deformity or abnormal appearance:
Fractured bone appears deformed, as the bone breaks and causes a significant misalignment. In some cases, the bone may pierce through the skin, which makes its deformity pretty obvious.
d) Inability to move or bear weight:
Bone fractures are extremely painful. The pain, combined with swelling and nerve damage, can restrict your movement. You won’t be able to lift weights or perform any physical activity until the bone gets back in shape.
Types of Fractures
Fractures are classified into different types based on the severity of the wound.
1) Simple vs. compound fractures:
In simple fractures, your bones crack but do not penetrate the skin. So, there’s no visible open wound. Compound fracture does penetrate the skin and requires immediate medical care.
2) Stress fractures:
It refers to a small crack in your bones caused by repetitive movements or overuse of your bones.
3) Greenstick and comminuted fractures:
Greenstick fractures are more likely to occur in children, as they have soft, flexible bones. The bone bends and cracks slightly without breaking completely. Comminuted fractures are more severe and are often caused by a serious fall or an accident. In this, the bone breaks into multiple pieces. You must see a fracture treatment doctor in Navi Mumbai if there’s a noticeable deformity combined with excruciating pain and a severe misalignment of the bones after an injury. Medical treatment is specifically required if the pain persists and you experience restricted movements.
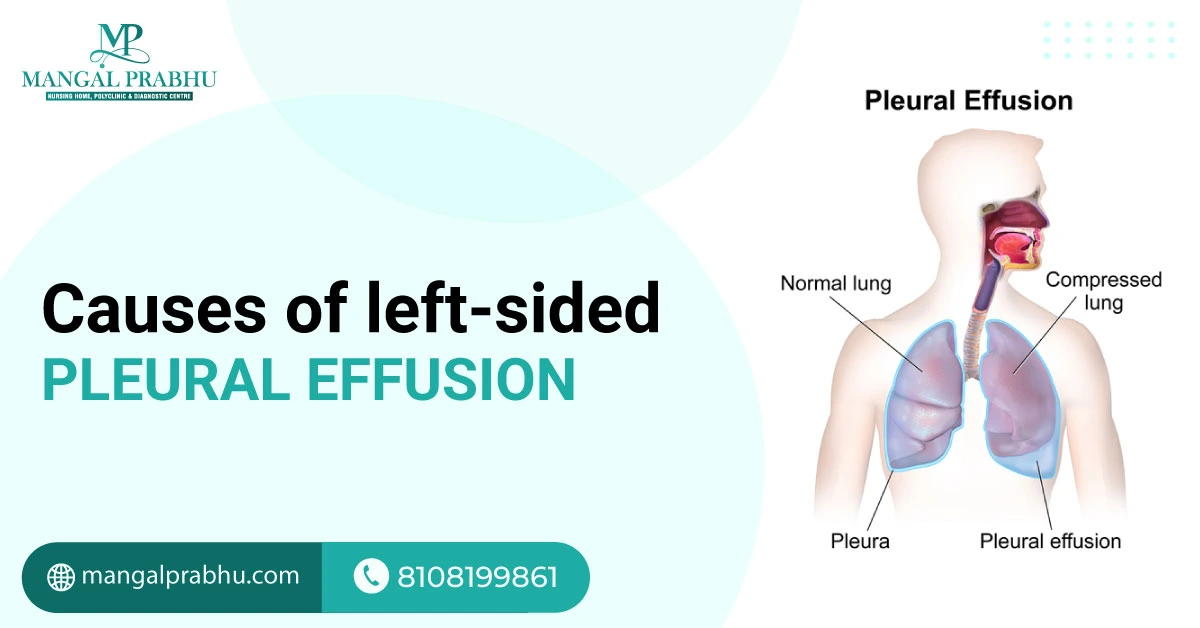
Causes of Left-sided Pleural Effusion
The pleura is described as a thin membrane lining the outside of your lungs and the chest walls. These naturally contain a small amount of fluid, which is produced to ensure smooth lung movements when you breathe. However, if a considerable volume of fluid is collected in the pleura cavity, it can indicate pleural effusion. A pulmonologist in Navi Mumbai will recommend medicine to fix it or a procedure that drains the excess fluid. Usually, the treatment focuses on identifying and treating the underlying cause.
Causes of Left-Sided Pleural Effusion
a) Heart-related Conditions:
Congestive heart failure is the common cause of left-sided pleural effusion. Your heart’s inability to pump blood sufficiently can lead to excess fluid accumulation in your pleural cavity. This is usually bilateral but can be one-sided. In some patients, pleural effusion occurs after cardiac surgery. Inflammation of the pleural cavity, an infection, or heart failure after surgery are the common causes.
b) Pulmonary conditions:
People with pneumonia and tuberculosis can develop pleural effusion. The infection can extend to the pleural cavity, filling it with fluid. Pulmonary embolism is another condition that increases the risk of pleural effusion. It happens when a blood clot gets into an artery in the lungs, causing a blockage. This blockage affects blood flow, resulting in fluid leakage into the pleural cavity.
Other Potential Causes
i) Trauma:
A serious heart injury that causes bleeding from the chest can lead to left-side pleural effusion.
ii) Autoimmune Diseases:
Your immune system can mistakenly attack your body’s tissues and organs. Lupus and rheumatoid arthritis are common examples of autoimmune diseases that can lead to pleural effusion.
iii) Cancer:
Lung cancer can cause fluid collection in the pleural cavity. Other cancers, like breast cancer or gastrointestinal cancer in their metastasis stage, can also spread to the pleural cavity, causing fluid buildup.
Diagnostic Approach
The healthcare provider will carefully examine your lungs at the pleural effusion treatment hospital in Navi Mumbai. They will ask about your symptoms and order imaging tests if needed.
A chest X-ray, for example, can show pleural effusion by highlighting the fluid in white while the rest of the space appears black. An ultrasound and CT scan might be needed to get a detailed picture of your chest and the pleural cavity. A minimally invasive procedure called thoracentesis is conducted to collect fluid samples from your pleural cavity using a catheter. This sample is sent to a lab for a thorough evaluation.
Treatment Options
Your doctor will address the underlying cause of the fluid buildup. If it’s caused by an infection, they will prescribe antibiotics to clear it. If it’s due to heart failure, diuretics might be used to reduce excess fluid from your body. Bronchodilators and NSAIDs can be used to help manage your symptoms. Thoracentesis is a medical procedure that involves inserting a needle into your pleural cavity to remove fluid and improve your breathing. Usually, treatment is decided based on the severity of the pleural effusion and its underlying cause.
What Causes Urine Blockage In Males?
An obstruction in any part of the man’s urinary tract can interrupt the normal urine flow. The blockage could be in the kidneys, which produce urine, or the urethra (responsible for releasing it). It’s important to see a urologist in Navi Mumbai if you suspect urine blockage, as an untreated obstruction can lead to uncomfortable symptoms, infection, and, in severe cases, kidney damage. The question is, what causes urine blockages in males? Let’s delve into some common reasons that might contribute.
What Causes Urine Blockage In Males?
1) Benign Prostatic Hyperplasia (BPH):
This is the most common cause of urine blockages in men. With age, the prostate gland that sits right beneath the bladder tends to get bigger. Its increased size can squeeze the urethra, affecting the urine flow. If your urinary obstruction is caused by BPH, you might also experience frequent urination, an inability to empty the bladder, and a weak or slow stream.
2) Kidney Stones:
These are hard mineral deposits that form in your kidneys and might travel down the ureters, causing an obstruction. These crystals can block the ureters (which carry urine to the bladder). The hallmark sign of kidney stones is debilitating pain in the back. Some people experience blood in the urine and nausea.
3) Urinary Tract Infections (UTIs):
UTI cases are more common in women, but men can also get this bacterial infection. It can block the urethra, disrupting the urine flow. If the blockage occurs due to UTI, you might notice cloudy urine, pain with a burning sensation while urinating, hematuria, and an uncontrollable urge to urinate.
4) Urethral Stricture:
Men who’ve had surgery or experienced a trauma that resulted in scar tissue formation in the urethra can also develop urine blockage. This happens due to the narrowing of the urethra due to scar tissue, inflammation, or an infection.
Symptoms and Diagnosis
Urinary obstruction can occur suddenly or gradually. Symptoms usually vary depending on the severity of the blockage. Here are some common symptoms people with a blocked urinary tract might experience:
- Difficulty starting to urinate
- Slow urine stream
- Frequent urge to urinate
- The feeling of unemptied bladder
- Pain during urination
- Blood in the urine
- Back pain
Treatment Options
Treatment of urinary obstruction in Navi Mumbai is determined based on what’s caused it. Here are a few options a urologist will discuss with you.
a) Medications:
Certain medications can help bring the prostate back to its normal size, although these may not always be effective. If you have a UTI, antibiotics can help clear the infection.
b) Surgical Interventions:
Surgery to widen the urethra may be necessary in case of urethral stricture. Surgery might also be needed in men with enlarged prostate or kidney stones that are too big to be removed naturally.
c) Lifestyle Changes:
A few lifestyle tips, such as limiting your caffeine and alcohol intake, drinking plenty of fluids, and peeing when you feel the urge to urinate, can help ensure optimal kidney function. See a urologist immediately if you experience a complete urinary tract obstruction with the inability to urinate.
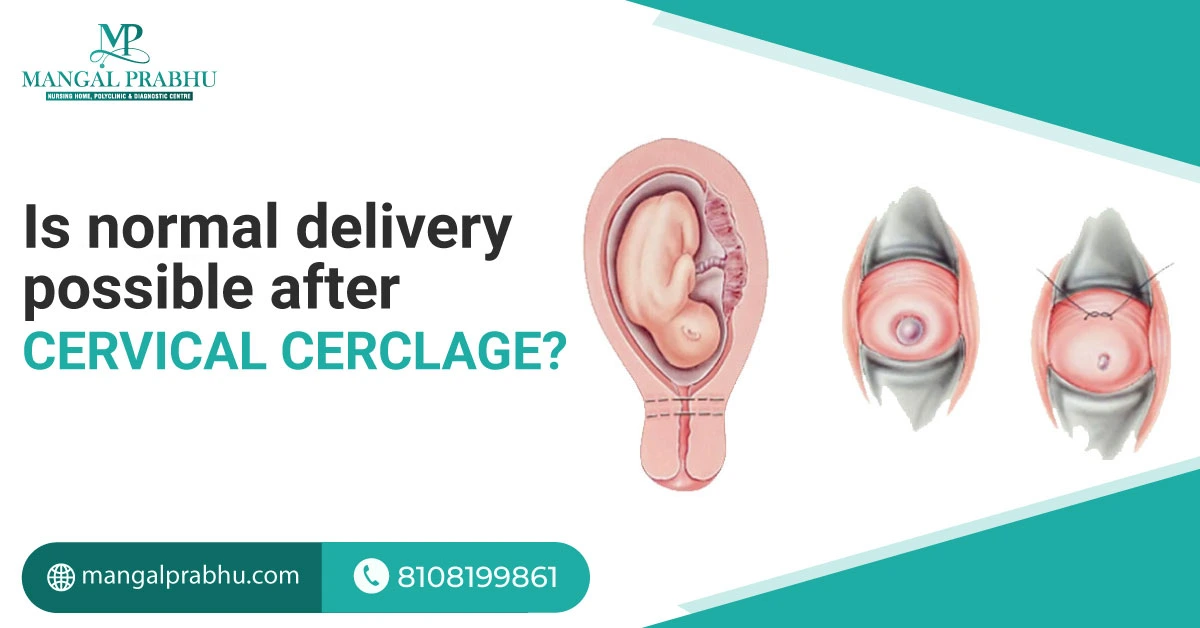
Is Normal Delivery Possible After Cervical Cerclage?
Cervical cerclage is done to prevent premature birth. Women who are at an increased risk of delivering a pre-term baby due to a weakened cervix might be offered this treatment. For women who are getting cervical cerclage, your biggest concern must be, “Is normal delivery possible after cervical cerclage”? Fortunately, yes. An obstetrician-gynecologist in Navi Mumbai might attempt normal delivery after removing cervical stitches. Here are more details about the procedure and the birthing options.
What is Cervical Cerclage?
Cervical cerclage refers to placing stitches on the cervix to keep it closed until you approach your delivery date. These will be removed when delivery is no longer considered premature. Your cervix is stitched when your doctor suspects a premature delivery because of an incompetent cervix, which is likely to open too soon, resulting in premature delivery.
The procedure is carried out around the second trimester and is mostly done on women with a history of pregnancy loss in the second trimester or a short cervix detected during an ultrasound.
Also Read : Most Common Cause of Vaginitis
Factors Influencing Delivery Method
Normal delivery is possible in women with a stitched cervix, although in a small percentage of cases, the healthcare provider recommends a c-section. Here’s what affects your delivery mode.
i) Cervix Health:
Your cervix needs to be intact and stabilized after cerclage removal if you want to attempt a vaginal delivery. Suppose the stitches weren’t removed already when you get into labor and the cervix tears. In that case, an immediate C-section delivery might be needed to prevent complications.
ii) Types of Cerclage:
Transvaginal cerclage, i.e., placing the stitches through the vagina, is the most common method of cerclage. Vaginal delivery is likely after transvaginal cerclage, as these can be removed before labor. Transabdominal cerclage, however, is a more complex procedure that involves stitching the cervix through your abdomen. In a transabdominal cerclage, the stitches remain in place, requiring a cesarean delivery.
iii) How Labor Progresses:
If labor progresses well and there’s no sign of an infection, fetal distress, or other complications, there’s a good chance you’ll deliver vaginally. If you experience pre-term labor, a c-section might be a safer bet.
Normal Delivery After Cervical Cerclage
You can talk to your doctor about a suitable time for a cervical cerclage removal surgery in Navi Mumbai to prepare yourself for vaginal birth. Once the stitches are removed and your cervix appears functional, you can opt for a normal delivery.
Potential Risks and Challenges
If the cervix is unable to maintain stability or strength for labor post-cerclage removal, cesarean delivery may be more appropriate. That’s because labor can cause cervical tears. There’s also a risk of infection around the surgical site, which can lead to complications during labor. Moreover, your doctor will remove cervical stitches around the 36th week of gestation, which might increase the chances of pre-term labor and birth. Vaginal delivery isn’t possible in cases with a history of multiple c-section deliveries. Your doctor will explain the risks and benefits of each delivery method, helping you make an informed decision.
Chicken pox Precautions For Family Members
What is Chickenpox?
With small red bumps all over the body and fever as its hallmark symptom, chickenpox is one of the highly contagious infections. It’s a common illness in children, but the symptoms, especially the red bumps that turn into blisters that eventually crust, can worry parents.
See a specialist for chicken pox treatment in Navi Mumbai if you notice its symptoms. It’s also important to be aware of the symptoms, how the infection spreads, and what precautions you can follow to protect your children from contracting varicella. Here’s all you should know.
Symptoms of Chickenpox
Exposure to the varicella-zoster virus can lead to chickenpox. Not every person with chickenpox requires treatment, though. You may recover fully within 1-2 weeks, although complications can arise in some cases.
These are some common symptoms of people affected by varicella:
- Low-grade fever (less than 102 °F)
- Fatigue
- Muscle ache
- Cough
- Headaches
- Stomach ache
- Loss of appetite
The most obvious sign of chickenpox is the rash that starts on the chest, back, belly, and face and spreads throughout the body. The rash becomes fluid-filled blisters. The blisters will turn into scabs. At this stage, the infected person won’t be contagious.
The above symptoms may last 3-5 days, and once you are fully recovered, you will develop immunity against the virus. People who are infected once are less likely to get it again.
How Does Chickenpox Spread?
As mentioned above, it’s a contagious disease that can spread easily. The risk of transmission is the highest in people who’ve never had chickenpox, unvaccinated people, and those with a compromised immune system.
The virus spreads when you come in contact with the infected person’s blister. It can also spread through coughing, sneezing, or touching contaminated surfaces.
Also Read: Types of Infectious Diseases
Chicken Pox Precautions For Family Members
1) Isolation:
To prevent transmission, you must keep the child with chickenpox in a separate room, preferably in a place where they’ve limited exposure to other children, elders, and people with weakened immunity. Isolation must be continued until all blisters have crusted.
2) Maintaining Hygiene:
Wash your hands thoroughly, as the infection spreads from touching contaminated surfaces. Sanitize your home, especially the areas touched frequently, like light switches, door knobs, mobiles, toys, books, etc.
3) Vaccination:
The vaccine for varicella-zoster virus is highly effective in preventing you from contracting the illness. Get vaccinated for chickenpox as soon as possible.
Managing Symptoms at Home
Some home measures can help speed up your recovery. Here’s what a general physician in Navi Mumbai recommends for faster recovery from the illness.
- Use a prescribed cooling lotion on the rashes for relief.
- Avoid itching or scratching, as these will worsen the infection.
- Take prescription drugs for controlling fever.
- Drink enough fluids to stay hydrated.
- Get enough rest
When To Seek Medical Care
If you develop a high-grade fever that persists for four days or longer and your rash becomes swollen and painful, seek immediate medical care. Other warning signs to watch out for include difficulty breathing, confusion, and seizures. Chickenpox might seem intimidating, but proper care and precautions will prevent transmission. The above tips will manage the illness and help with speedy recovery.

How to Prevent Jaundice in Newborns?
Welcoming a new human into the world might be the most exciting yet overwhelming moment for parents. Caring for your little bundle of joy requires patience and dedication. A common issue that makes parents worry is newborn jaundice. It’s a medical condition that turns the whites of the eye and the skin yellow due to the high amount of bilirubin in the bloodstream.
It’s quite common in pre-term babies and is often manageable. In some cases, you may need neonatal jaundice treatment in Navi Mumbai. In this post, we’ll explain early signs of jaundice, how to protect your newborns, and when medical attention is necessary. Keep reading.
Understanding Jaundice
Neonatal jaundice occurs when the baby’s immature liver doesn’t filter excess bilirubin in the blood efficiently. Bilirubin is a waste product of red blood cells. Normally, bilirubin is released into a person’s intestinal tract, from where it’s excreted through urine and stools. That’s, however, not the case with newborns.
Their red blood cells break down faster than those of adults, causing excessive bilirubin levels. This, combined with their liver’s inability to process this yellow pigment effectively, makes them more prone to jaundice than adults. The good news is that, in most cases, newborn jaundice isn’t a cause for concern. It resolves within a few days without treatment. Rarely, an extreme amount of bilirubin in blood can lead to brain damage.
Early Detection
If your baby has jaundice, you must monitor their symptoms and call a pediatrician in Navi Mumbai if they persist or worsen. Here are the common symptoms of newborn jaundice:
- Yellowing of the eyes and the skin
- Dark urine
- Drowsiness or difficulty waking up
- Not feeding well
To know if your baby has jaundice, slightly press their skin. If it changes its color to yellow, it might indicate an excess bilirubin. Pre-term babies are at an increased risk, as their bodies might not adjust to the outside world as well as that of a term baby. Besides, they may have difficulty feeding, affecting their urine and bowel output. This, in turn, leads to less bilirubin removed from their body.
Preventative Measures
Here are some preventive measures that can protect your newborn from jaundice.
i) Regular Feeding:
In the first few weeks, infants must be fed 8-12 times daily. Formula-fed babies must also be fed every 2-3 hours, depending on how often they demand it. Babies who are dehydrated or do not get sufficient nutrients from breast milk can develop jaundice.
ii) Breastfeed:
Breastmilk, especially colostrum (the first milk), is a rich source of nutrients that help a baby’s growth. It also acts as a natural laxative, which helps in excretion. If your baby gets enough colostrum, they are less likely to have jaundice.
iii) Sunlight Exposure:
Sunlight helps break down excess bilirubin in the baby’s skin. So, aim to give your baby indirect sunlight. That said, phototherapy is a more practical alternative.
Medical Interventions
If the baby’s bilirubin level rises above 15 mg/dL and is accompanied by poor feeding and lethargy, take them to a pediatrician immediately. They will recommend phototherapy or blood transfusion in severe cases. Make sure timely treatment can save your baby from complications like brain damage.

Functions of Emergency Department in Hospital
Critical medical conditions that require immediate medical attention can strike at any time. Anyone can become the victim of unexpected illnesses or accidents that can be life-threatening if not treated promptly. That’s when the multispecialty hospital in Navi Mumbai, equipped with an emergency department, comes to your rescue.
The department doesn’t just have advanced medical devices that monitor the patient’s vitals round-the-clock, but these are staffed 24/7 by professionals who offer premium care to the patient. So, what exactly are the functions of the emergency department in the hospital? Let’s find out.
Functions of Emergency Department in Hospital
Primary Functions
When a patient is admitted to the emergency room, it’s mainly because of a life-threatening condition that can result in severe complications or possibly death in most cases. This includes patients who’ve suffered a heart attack, a severe injury to their vital organs, or breathing difficulties. After admission, the doctors will carefully assess the root cause of the issue and focus on stabilizing your health, ensuring that your vitals are controlled, you are not in pain, and you won’t suffer further deterioration.
A Triage
An emergency care hospital in Navi Mumbai follows a triage system in which patients are sorted by the severity of their condition. Those who have a critical medical issue get immediate attention. Patients who can survive without advanced life support are admitted to the general ward or private rooms (based on their preference). The system ensures that patients with severe medical issues, such as cardiac arrest or trauma, are given emergency care to save their lives.
Coordination with Specialized Departments
A multispecialty hospital is staffed with doctors specializing in different segments of the healthcare industry. These hospitals have neurosurgeons, cardiologists, pediatricians, gynecologists, and other specialists who can offer immediate care and surgery if needed. Depending on the case, the patients might be referred to another hospital that’s staffed with specialists in the particular area of medicine.
Challenges Faced
1) Stressful Decisions:
Specialists working in the emergency department often have to make critical decisions, such as whether it’s worth keeping the patient on life support or not. Besides, the life-threatening illnesses that sometimes lead to death can be super overwhelming for doctors.
2) Switching Jobs:
Healthcare professionals must be qualified to perform various invasive and non-invasive treatments for different cases. One minute, they may be handling an emergency gynecology surgery to repair a ruptured fallopian tube, and the next, they may be performing an emergency kidney transplant. This can make their jobs challenging.
3) Technological Challenges:
Not every emergency department in a multispecialty hospital is equipped with advanced technological tools to handle emergency cases effectively. Besides, overcrowding may result in a shortage of hospital beds and rooms to admit critically ill patients.
Conclusion
There’s no denying that emergency units make hospitals the “safe place” for people who’ve sustained an unexpected injury or medical crisis. The key players are qualified doctors who do their best to keep the patient alive, stabilize their vitals, and ensure that their condition is normal. Besides that, high-quality, technologically advanced tools used in these facilities offer the best life support.
What are the Stages of Typhoid Fever?
Typhoid fever is a critical, contagious illness that occurs when the bacteria “Salmonella Typhi” enter your system and multiply within the bloodstream and intestines. People living in places where poor sanitation practices are followed are prone to contracting the illness.
It’s important that you know the different stages of typhoid fever, how it spreads, and, more importantly, prevention steps to minimize your risk of getting typhoid. If you suspect typhoid, seek immediate medical care from a General Physician in Navi Mumbai to reduce your risk of complications. In this post, we’ll walk you through the early and advanced stages of typhoid. Let’s take a look:
What are the Stages of Typhoid Fever?
Stage 1: Early Symptoms
The symptoms of typhoid aren’t noticeable in most cases during the incubation period or the early stage of the disease. This can start in the first few days of contracting the bacteria or up to 60 days. The severity of this contagious illness depends on your immunity and the bacterial strain ingested.
Stage 2: Acute Illness
Symptoms show up during this phase. As it progresses, you will notice high-grade fever, often spiking to 104°F, accompanied by muscle aches, fatigue, headache, and loss of appetite. The acute stage of typhoid fever can last for days and can lead to complications if left unaddressed for a long time. The symptoms start with a mild fever, which progresses gradually. Remember, the gradually increasing temperature and persistent fever are key indicators of typhoid.
Stage 3: Peak of Infection
If your doctor starts antibiotics during the acute phase, the symptoms will subside, and you’ll feel better. However, if the treatment isn’t started, the symptoms might worsen due to the bacteria spreading to the bloodstream and intestines. Some people report constipation, while others experience diarrhea. Abdominal pain is also common at this stage. You might experience difficulty concentrating due to the high-grade fever.
If you experience these symptoms, especially if your temperature doesn’t drop, visit the nearest hospital for typhoid treatment in Navi Mumbai. Delayed treatment can increase the risk of complications, including intestinal bleeding and septic shock.
Stage 4: Recovery
Also called the Convalescence stage, your body goes into the recovery phase. Your immune system fights off the infection, which may help subside the fever and manage other symptoms. Still, some patients report muscle aches, fatigue, and weakness for several weeks after the acute phase.
It’s important to follow your doctor’s advice and complete your course of antibiotics, even if the symptoms have subsided. Skipping medication can lead to the bacteria resurfacing.
Prevention Tips
To help mitigate the risk of typhoid, we have listed a few preventive measures that can help.
- Make a habit of washing your hands thoroughly before eating.
- Carry bottled water or boiled water when traveling.
- Avoid high-risk areas, especially if you have weak immunity.
- Vaccination is also available for those with an increased risk of contracting typhoid.
- Never eat veggies and fruits without washing them.
Conclusion
The symptoms of typhoid are often confused with flu and common cold. That’s why many people do not visit the hospital until the condition worsens and the fever doesn’t subside. The earlier you seek medical care, the better your chances of recovering quickly.

How Does Cancer Spread?
What makes cancer life-threatening is its ability to spread to the major organs. No matter where it started, it can travel through your bloodstream or lymph nodes and invade your vital organs. In medical terms, the process is called metastasis. An oncologist in Navi Mumbai provides cancer patients with an accurate diagnosis and a suitable treatment plan.
Simply put, cells from the tumor escape and enter your blood, transporting them to different parts of your body. Research regarding “how does cancer spread” is still going on. The more we know about the process, the more treatment options we can explore for a higher success rate.
How Does Cancer Spread?
Metastasis is a complex process. It starts with local invasion, in which the cancer cells break away from the tumor (in the primary site) and enter the nearby tissues.
From there, they find their way into your bloodstream and lymphatic system. That’s called intravasation. Your immune system kills most cancer cells at this stage, but a few might escape and settle in a new location. They form a secondary tumor there.
Common Sites for Metastasis
The areas invaded by the cancer cells depend on where the cancer starts. For example, cancer starting in the breast will travel to the lymph nodes of your underarms rather than your abdomen.
It also depends on the cancer cell type. These cells tend to settle in locations where they can thrive. Prostate cancer cells prefer your bones, as they offer these cells the environment to grow and spread. Here are the common locations for cancer cells to spread:
- Bladder cancer: Bones, lungs, or liver
- Breast cancer: Brain, liver, and lungs
- Prostate cancer: Bones, liver, lungs
- Lung cancer: Bones, brain, and liver
Most types of cancers spread to the lungs, liver, bones, and brain.
Detection and Diagnosis of Metastatic Cancer
Some cancers are detected when metastasized—already spread to other organs. Here’s the list of tools used for diagnosing metastatic cancer.
a) Imaging Techniques:
CT scans, ultrasounds, MRIs, bone scans, and PET scans are imaging tests that locate cancer cells and show their extent of spread.
b) Biopsy:
If malignancy is suspected, your doctor might extract sample tissues and send them to the lab for testing. These cells are tested for tumor markers or abnormal growth.
Treatment Options for Metastatic Cancer
A cancer Hospital in Navi Mumbai will discuss treatment options based on the originating site of the cancer, where it has spread, and your symptoms. Depending on the location, an oncologist might start with chemotherapy and radiation therapy.
In some cases, these are used in conjunction with hormonal therapy and immunotherapy. These treatment options are designed to kill cancer cells or slow their growth. In some cases, surgical removal of the tumor that has invaded a vital organ may be necessary.
Conclusion
Metastatic cancer, in most cases, is not curable, which is why early detection of cancer is key to a successful treatment. Treatment of metastatic cancer usually focuses on managing symptoms. That said, technological advancements have encouraged professionals to explore new treatment options and therapies to improve patient’s survival rates and quality of life.
